Introduction
How far are we willing to go in pursuit of society’s elusive thin ideal?
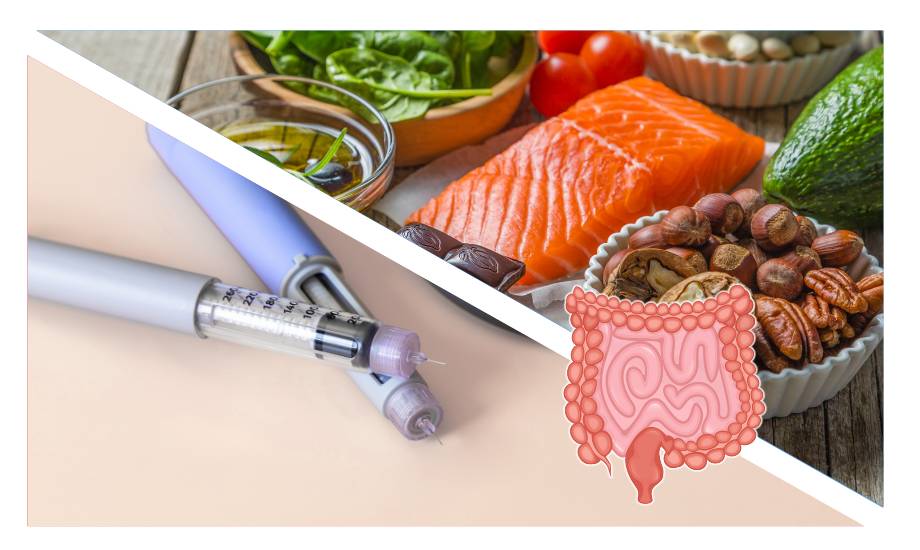
The relentless pressure to conform to narrow standards of beauty has driven many individuals to extreme measures, including the use of GLP-1 drugs like Ozempic, in hopes of achieving rapid weight loss and acceptance. However, amidst the allure of shedding pounds and attaining the coveted silhouette lies a lesser-known reality: the potential consequences for gut health. While these medications may offer a temporary solution to the pressures of our image-obsessed culture, their impact on the delicate balance of the gut microbiome cannot be ignored. In the quest for thinness, are we sacrificing our gut health at the altar of societal expectations?
While Ozempic may offer a temporary reprieve from the pressures of our image-obsessed culture, its impact on gut health cannot be ignored. As the delicate ecosystem of bacteria within our intestines reels from the onslaught of pharmaceutical intervention, the consequences reverberate far beyond the confines of a bathroom scale. From digestive distress to immune dysfunction, the toll of disrupting the delicate balance of the gut microbiome can be profound and far-reaching.
In our relentless pursuit of the thin ideal, let us not forget the inherent beauty and resilience of the human body—a vessel not defined by its size, but by its strength, vitality, and capacity for growth. As we navigate the complexities of weight loss and wellness, may we strive for a harmony that transcends societal expectations and embraces the intrinsic worth of every individual, regardless of the numbers on a scale or the shape of a silhouette.
Understanding GLP-1
What is GLP-1?
Glucagon-like peptide-1 (GLP-1) is a hormone produced in the gut in response to food intake. Its primary role is to regulate glucose metabolism and promote satiety. When food enters the digestive system, GLP-1 is released, stimulating insulin secretion, inhibiting glucagon release, slowing gastric emptying, and promoting feelings of fullness.
Mechanism of Action of GLP-1 Drugs
Targeting GLP-1 Receptors
GLP-1 drugs such as Ozempic belong to a class of medications known as GLP-1 receptor agonists. These drugs are designed to mimic the activity of naturally occurring GLP-1, a hormone produced by specialized cells in the lining of the intestine called L-cells.
Amplifying Physiological Responses
Upon activation, GLP-1 receptors initiate a cascade of physiological responses aimed at regulating glucose metabolism and appetite. One of the primary actions of GLP-1 is to stimulate the release of insulin from pancreatic beta cells in response to elevated blood sugar levels. This insulin release helps to lower blood glucose levels, promoting glycemic control.
Slowing Gastric Emptying
In addition to its effects on insulin secretion, GLP-1 slows down the rate at which food is emptied from the stomach into the small intestine, a process known as gastric emptying. This delay in gastric transit has several implications on metabolism and appetite. By prolonging the time it takes for food to leave the stomach, GLP-1 drugs increase feelings of fullness and reduce appetite, leading to decreased food intake and ultimately, for many, weight loss.
Promoting Satiety
Furthermore, GLP-1 receptor activation enhances satiety signals in the brain, signaling feelings of fullness and satisfaction after a meal. This satiety-promoting effect reduces cravings and overall decreases appetite.
Preserving Beta Cell Function
Beyond its immediate effects on glycemic control and appetite regulation, GLP-1 receptor agonists like Ozempic have also been shown to exert beneficial effects on pancreatic beta cell function. Beta cells are special cells in the pancreas that make insulin, a hormone that helps control sugar levels in the blood. By promoting the survival and proliferation of beta cells, these medications help to preserve insulin-producing capacity in individuals with type 2 diabetes, further supporting long-term glucose regulation.
In summary, GLP-1 drugs like Ozempic exert their therapeutic effects by activating GLP-1 receptors in the gut, leading to a coordinated response aimed at improving glycemic control, impacting appetite and gastric emptying, and preserving pancreatic function. This multifaceted approach has made them a tool in the management of type 2 diabetes.
Too good to be true?
GLP-1 drugs have revolutionized the treatment landscape for type 2 diabetes, offering a powerful tool for managing blood sugar levels and reducing the risk of complications. However, their benefits extend beyond diabetes management, as they have also emerged as weight loss aids. But does it come without consequences?
Despite their efficacy in promoting weight loss, GLP-1 drugs like Ozempic have brought with them some unintended consequences, particularly concerning gut health. As users chase the promise of rapid weight loss, the impact of these medications on the delicate balance of the gut microbiome has become increasingly apparent, raising concerns about potential long-term effects on digestive function and overall health.
Impact on Intestinal Peristalsis
Modulating Gut Motility
One significant impact of GLP-1 receptor agonists like Ozempic is their effect on intestinal peristalsis—the wave-like contractions that propel food through the digestive tract. By slowing gastric emptying, GLP-1 drugs prolong the time it takes for food to move through the stomach and intestines. This delay in gastric transit contributes to increased feelings of fullness and reduced appetite, therefore typically resulting in decreased caloric intake.
Delayed gastric emptying
The delay in gastric emptying caused by GLP-1 receptor agonists like Ozempic can have downstream effects on digestion, potentially leading to unwanted impacts such as dysbiosis and small intestinal bacterial overgrowth (SIBO). When food lingers in the stomach and intestines for longer periods, it creates an environment that is conducive to the overgrowth of certain bacteria.
This imbalance in gut microbiota, known as dysbiosis, can disrupt normal digestive processes and contribute to symptoms such as bloating, gas, and abdominal discomfort. Additionally, the prolonged presence of undigested food in the small intestine may promote the growth of bacteria in this region, leading to SIBO—a condition characterized by an overgrowth of bacteria in the small bowel.
SIBO can interfere with nutrient absorption and cause symptoms such as diarrhea, constipation, and nutrient deficiencies.
Therefore, while GLP-1 drugs like Ozempic offer benefits for weight management, their effects on gastric emptying may have unintended consequences for gut health and digestive function, highlighting the importance of monitoring and addressing potential gastrointestinal issues in individuals undergoing treatment.
Influence on Microbiota Composition
Shaping the Gut Ecosystem
Emerging research suggests that GLP-1 receptor agonists may also influence the composition and function of the gut microbiota—the diverse community of bacteria residing in the gastrointestinal tract. Studies have shown that alterations in gut motility and nutrient availability induced by GLP-1 drugs can impact microbial populations, leading to shifts in microbiota composition.
Other bacterial taxa may experience a reduction in abundance in response to GLP-1 receptor agonist therapy. These changes in microbial composition could have downstream implications for digestive health, immune function, and metabolic regulation. Additionally, shifts in the gut microbiota composition may contribute to the observed effects of GLP-1 drugs on appetite regulation, energy metabolism, and weight management.
Balancing Act
While GLP-1 drugs like Ozempic offer promising benefits for weight management and glycemic control, their impact on the gut microbiome raises important considerations. Disruptions to microbial diversity and function have been linked to various health conditions, including metabolic disorders and immune dysregulation. Thus, achieving a balance between the therapeutic effects of GLP-1 agonists and preserving gut health is essential for long-term wellness.
Gut Bacteria that impact GLP-1
Akkermansia muciniphila
While the direct mimicry of Ozempic’s action by specific gut bacteria remains elusive, research has uncovered correlations between certain bacterial strains and metabolic effects akin to those induced by Ozempic. For instance, studies have observed an increase in the abundance of bacteria such as Akkermansia muciniphila—a microbe associated with improved metabolic health and a lean phenotype—in individuals treated with GLP-1 receptor agonists. Akkermansia muciniphila plays a vital role in maintaining the integrity of the gut barrier and metabolizing mucin, a key component of the protective mucus layer lining the intestinal wall. By bolstering levels of Akkermansia muciniphila, GLP-1 drugs may confer benefits for gut health and metabolic function.
Bacterial diversity in the gut
Furthermore, the overall diversity and composition of the gut microbiome may indirectly influence GLP-1 production and signaling in the gut, thereby impacting various metabolic processes relevant to weight management. A diverse and balanced microbiome is crucial for maintaining gut health and facilitating proper nutrient absorption. Dysbiosis, characterized by an imbalance in microbial communities, can disrupt normal gut function and impair metabolic processes. In this context, alterations in the gut microbiota composition may affect GLP-1 production and signaling pathways, potentially influencing appetite regulation, energy metabolism, and glucose homeostasis.
Understanding the intricate interplay between gut bacteria, GLP-1 signaling, and metabolic health is essential for elucidating the broader implications of gut microbiome modulation in the context of weight management and metabolic disorders. While specific bacterial strains may not directly replicate the actions of Ozempic, their presence and abundance within the gut ecosystem contribute to the complex network of interactions that shape metabolic health outcomes. Further research into the mechanisms underlying these relationships holds promise for identifying novel therapeutic targets and interventions aimed at harnessing the therapeutic potential of the gut microbiome in the treatment of metabolic conditions.
Overall, while GLP-1 receptor agonists like Ozempic hold promise for improving metabolic health, their impact on the gut microbiota underscores the need for further research into the complex interplay between pharmaceutical interventions, gut microbiome dynamics, and overall health outcomes. By gaining a deeper understanding of how GLP-1 drugs shape the gut microbiota, researchers can explore innovative strategies to optimize therapeutic benefits while minimizing potential risks associated with microbiome alterations.
How to naturally increase GLP-1 in your gut
Maintaining a healthy gut is essential for overall well-being, and one of the key players in this process is GLP-1 (Glucagon-like peptide-1). This hormone helps regulate blood sugar levels, promotes feelings of fullness, and supports weight management. While many people turn to medications like Ozempic to boost GLP-1 levels, there are also natural ways to enhance its production through diet. By incorporating certain foods into your daily meals, you can naturally stimulate GLP-1 production and improve your gut health. Here are 10 practical and delicious additions to your diet that can help increase GLP-1 in the gut, without the need for restrictive eating.
While the direct mimicry of Ozempic’s action by specific gut bacteria remains elusive, research has uncovered correlations between certain bacterial strains and metabolic effects akin to those induced by Ozempic. For instance, studies have highlighted the association between increased abundance of particular bacterial species, notably Akkermansia muciniphila, and enhanced metabolic health outcomes. Akkermansia muciniphila, a mucin-degrading bacterium residing in the mucus layer of the gut, has garnered significant attention for its potential role in metabolic regulation. Research suggests that higher levels of Akkermansia muciniphila are linked to improvements in glucose control, reduced inflammation, and protection against metabolic-related complications.
Furthermore, the overall diversity and composition of the gut microbiome may indirectly influence GLP-1 production and signaling in the gut, thereby impacting various metabolic processes relevant to weight management. A diverse and balanced microbiome is crucial for maintaining gut health and facilitating proper nutrient absorption. Dysbiosis, characterized by an imbalance in microbial communities, can disrupt normal gut function and impair metabolic processes. In this context, alterations in the gut microbiota composition may affect GLP-1 production and signaling pathways, potentially influencing appetite regulation, energy metabolism, and glucose homeostasis.
How to naturally increase GLP-1 in your gut
Understanding the intricate interplay between gut bacteria, GLP-1 signaling, and metabolic health is essential for elucidating the broader implications of gut microbiome modulation in the context of metabolic health. While specific bacterial strains may not directly replicate the actions of Ozempic, their presence and abundance within the gut ecosystem contribute to the complex network of interactions that shape metabolic health outcomes. Further research into the mechanisms underlying these relationships holds promise for identifying novel therapeutic targets and interventions aimed at harnessing the therapeutic potential of the gut microbiome in the treatment of metabolic conditions.
1. Eat More Fiber-Rich Foods
Fiber-rich foods like fruits, vegetables, legumes, and whole grains help stimulate the production of GLP-1. They slow down digestion and provide a steady release of nutrients, which can enhance GLP-1 secretion.
2. Include Fermented Foods
Fermented foods such as yogurt, kefir, sauerkraut, kimchi, and kombucha contain beneficial probiotics that can support gut health and potentially increase GLP-1 levels.
3. Add Resistant Starch
Foods high in resistant starch, such as green bananas, cooked and cooled potatoes, and legumes, can boost the production of short-chain fatty acids (SCFAs) in the gut, which may help increase GLP-1 secretion.
4. Consume Healthy Fats
Incorporate healthy fats like avocados, nuts, seeds, and olive oil into your diet. These fats can enhance the release of GLP-1 by slowing down gastric emptying and promoting satiety.
5. Eat Protein-Rich Foods
Proteins from lean meats, fish, eggs, dairy, and plant sources like beans and lentils can stimulate GLP-1 release. Aim to include a source of protein with each meal (ideally 20-30 grams if possible).
6. Include Omega-3 Fatty Acids
Foods high in omega-3 fatty acids, such as fatty fish (salmon, mackerel, sardines), chia seeds, flaxseeds, and walnuts, may help enhance GLP-1 levels and improve overall gut health.
7. Add Spices and Herbs
Spices like turmeric and ginger have anti-inflammatory properties and may support the production of GLP-1. Adding these to your meals can enhance flavor and health benefits.
8. Consume Polyphenol-Rich Foods
Polyphenol-rich foods, such as berries, dark chocolate, green tea, and red wine, can support gut health and may help increase GLP-1 production. These foods also offer antioxidant benefits.
9. Drink Green Tea
Green tea is rich in catechins, which are antioxidants that can support gut health and potentially increase GLP-1 levels. Enjoy a cup of green tea daily for these benefits.
10. Eat Prebiotic-Rich Foods
Prebiotic foods like garlic, onions, leeks, asparagus, and Jerusalem artichokes feed beneficial gut bacteria, supporting a healthy microbiome that can enhance GLP-1 production.
By incorporating these foods into your diet, you can naturally support the production of GLP-1 in the gut, promoting better metabolic health and aiding in weight management.
Conclusion
By delving into the mechanisms of GLP-1 action and its effects on intestinal peristalsis and microbiota composition, we gain a deeper understanding of how medications like Ozempic interact with the body and the potential implications for overall health and well-being.
Remember that this blog is not a substitute for medical advice. Please consult your healthcare provider before trying anything new.